“I’m not trying to talk down to you,” said Travis Campbell from his hospital bed. “I’m trying to talk to you so you understand that I don’t want to go to your funeral and I don’t want you to come to mine.”
As Covid-19 cases surge in parts of the country with low vaccination rates, driven by the highly contagious Delta variant, stories of unvaccinated Americans expressing deep regrets from their deathbeds are spreading across social media, with healthcare workers facing the excruciating task of telling some patients that it’s too late to help them.
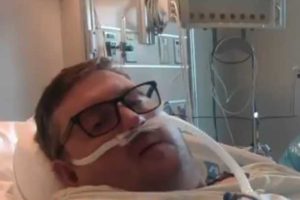
On Friday CNN reported the story of Travis Campbell, who has been in a hospital in Virginia for two weeks battling Covid-19—which has caused him to develop pneumonia and left him with a partially collapsed lung—after putting off getting vaccinated not because of stubborn “vaccine hesitancy,” but due to a move and knee surgery.
“I messed up big time, you guys—I didn’t get the vaccine,” 43-year-old Campbell said in a video he posted to Facebook on Wednesday in hopes of convincing people in his circle to get vaccinated.
“I’m so sorry that I made the mistake to not get vaccinated. Vaccinations are so important, and I can do better as a parent, as a human, and I hope to god everybody else can, too.”
Travis Campbell, who is in the hospital with Covid-19, says he regrets not taking the vaccine. pic.twitter.com/mQKx0I0j4F
— CNN (@CNN) August 6, 2021
Campbell’s story follows that of Micheal Freedy, who was not opposed to vaccination in general but wanted to wait until the vaccines had been available for a year to ensure they were safe, and who texted his fiancee, “I should have gotten the damn vaccine” from an intensive care unit in a Las Vegas hospital last month before succumbing to the illness.
Campbell’s illness and Freedy’s death are just two illustrations of the crises healthcare workers are coping with in areas with low vaccination rates, particularly across the South.
Dr. Thomas Dobbs, the state health officer for Mississippi—where the vaccination rate is the lowest in the country, with 44.3% of people fully inoculated—told reporters on Thursday that the Delta variant is “sweeping across [the state] like a tsunami,” accounting for 90% of new cases and packing intensive care units even in children’s hospitals.
The state reported more than 3,000 new cases in a single day on Thursday. In neighboring Louisiana, officials are currently reporting a daily average of 4,300 cases—the highest per capita rate of cases in the country. Just over 47% of Louisiana residents are vaccinated, according to the New York Times, but fear of the Delta variant has reportedly pushed more people to sign up for vaccinations in recent weeks.
The Times reported that demand for the shots has nearly quadrupled in recent weeks amid reports that unvaccinated people in their 20s and 30s are becoming seriously ill and even dying.
“The public is finally hearing how bad it has gotten,” Dr. Robert C. Peltier, the chief medical officer for North Oaks Health System near Baton Rouge, told the Times.
Campbell is among those who are now trying to use their personal experiences to urgently persuade others to get vaccinated without approaching them in anger.
“I’m not trying to talk down to you. I’m trying to talk to you so you understand that I don’t want to go to your funeral and I don’t want you to come to mine,” Campbell said in the video he posted. “The new delta strain … will get you down so fast you are not going to get back up.”
Campbell’s tone is a far cry from some politicians who have accused unvaccinated people of “letting us down,” as Alabama Gov. Kay Ivey did in recent weeks. Ivey, a Republican, initially expressed skepticism about public health measures when the pandemic began.
Widespread anger over people’s hesitancy to get vaccinated—due to misinformation or other reasons—has given way to harsh approaches by policymakers as they resort to punishing those who haven’t yet.
Economist Justin Wolfers and Sen. Brian Schatz (D-Hawaii) have both floated the possibility of charging people more for health insurance—a proposal denounced as “not only cruel but reckless” by Natalie Shure at The New Republic on Friday.
While vaccine mandates, like the one introduced in New York City this week, have been shown to be effective—successfully increasing vaccination rates by 40% in New York after Mayor Bill de Blasio announced the rule—they have “appreciable limits,” Shure wrote:
Even in liberal strongholds like New York City, mandates have sparked protest, such as SEIU 1199’s demonstration in front of New York Presbyterian Hospital. But that’s nothing compared to the political hostility marshaled against mandates in more conservative areas—which are often places with comparatively low vaccination rates that ostensibly need mandates the most.
[…]
All of this points to a frustrating fact about vaccine mandates: You can’t lean too hard on them simply because you’re throwing in the towel on persuasion, because the same political and social forces that result in low vaccination rates also make mandates less feasible. And where mandates are implemented, their effectiveness will still rely on broad social support.
In the Times on Friday, columnist Bryce Covert wrote about efforts to make vaccines more accessible by deploying mobile clinics at community gatherings and reaching out in practical ways to people facing food insecurity—as unvaccinated people are three times as likely to be—or people who have difficulty taking time away from work to get a shot.[content id=”79272″]
“Missing out on a few hours of work seems very easy to us, but in fact it could be the matter of having food for the family versus not,” Ann Lee, chief executive of the nonprofit Community Organized Relief Effort, told Covert. “The wages are going to win out.”
To make vaccination more practical and enticing to people, Covert wrote, organizers in communities across the country have turned not to mandates but vaccine drives at public housing complexes, construction sites, and fields where agricultural laborers work long hours.
“They wanted to get vaccinated. There was just no way some of these day laborers were going to take off of work and maybe get sick,” Lee said.
Shure suggested frustrated, vaccinated Americans direct their anger at “a Congress that held up state and local vaccination funding for months, to such a degree that the money only reached public health departments in early February—months after the vaccine debuted.”
The funding lag has made it more difficult for officials in many parts of the country to implement “creative, proactive strategies that bring ease, accessibility, and ubiquity to the cause,” Shure wrote, “which could reach people who are just beyond the reach of institutions and outside the grasp of any mandate.”
Common Dream’s work is licensed under a Creative Commons Attribution-Share Alike 3.0 License. Feel free to republish and share widely.
[content id=”79272″]